Neurological Examination and Assessment
During spinal cord injury primary and secondary examinations neurological examinations are carried out to assess the severity and location of damage to the spinal cord. These examinations aim to provide information on the neurological level of spinal cord injury, extent of injury to the spinal cord, and the resulting degree of impairment. Performed upon initial hospitalization and repeated periodically during rehabilitation, the collated results assist in determining how much support may be required upon discharge from hospital. For initial assessment purposes a typical neurological examination where spinal cord injury is suspected will include the following tests;
- Cranial nerve function: There are 12 cranial nerves which are nerves that originate in the head, coming off the brain and brain stem. The examination of these nerves and their functions is complex but includes areas such as smell, vision and eye movements, facial sensation, reflexes and movement, hearing, taste, tongue and palate movements and even movements of the head, neck and shoulders.
- Power of muscle groups according to the Medical Research Council scale: This part of the examination tests the motor function, or movement, of the major muscle groups, most notably in the shoulders, arms, hips and legs. The muscles are tested for mass, muscle tone, and strength.
- Reflexes including abdominal, anal, and bulbospongiosus: Various reflexes are tested throughout the body. While these can indicate problems with sensation and/or motor function, they can also reveal other aspects of nervous system dysfunction as well.
- Sensation to pin prick, fine touch and joint position sense: The sensory exam part of the neurological exam evaluates the sensation of the patient. This includes not just normal touch but also pain and temperature and sensation of limb position and movement.
Detailed neurological examinations may include CAT, IVP and MRI scans, a cerebral angiogram, electroencephalogram, electromyogram, and nerve conduction study.
Myotomes and Dermatomes
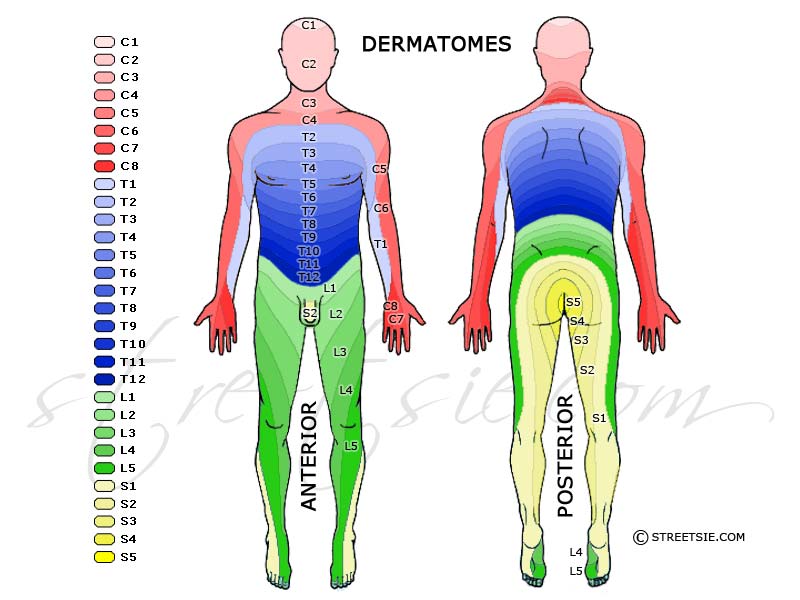
Each myotome (muscle) and dermatome (region of skin) of the body is supplied by a particular level or section of the spinal cord and by its corresponding spinal nerve. There are eight cervical nerves, twelve thoracic nerves, five lumbar nerves and five sacral nerves. Each of these nerves relays sensation (including pain) from a particular muscle or region of skin to the brain. By examining the dermatomes and myotomes this way, a motor score, level and completeness of a spinal cord injury can be determined.
According to the American Spinal Injury Association (ASIA) standard neurological classification guide the last dermatome or region of skin with healthy intact sensation displaying normal spinal cord function is considered the neurological level of injury. This does not necessarily correspond with the vertebral (spinal column bone or disc) level of injury. Therefore both neurological and vertebral diagnoses are recorded. Additionally while the following muscles grades are not included in determining the ASIA motor score and level they should still be assessed and noted.
- Diaphragm – C3,4,5
- Shoulder abductors – C5
- Supinators/pronators – C6
- Wrist flexors – C7
- Finger extensors – C7
- Intrinsic hand muscles – T1
- Hip adductors – L2,3
- Knee flexors – L4,5 S1
- Toe flexors – S1, S2
Neurological Level of Spinal Cord Injury
A significant proportion, 55% of cases admitted to spinal units involve the cervical segments C1-C7. This type of impairment is referred to as tetraplegia (or quadriplegia). Injury at the thoracic, lumbar or sacral levels, are referred to as paraplegia. In Australia over the past eight years cervical spine injuries have accounted for between 50% and 59% of all SCI. The most common cervical spine injuries involved C4-C5. This group accounted for 61% of cervical SCI cases and 32% of all 241 documented neurological injuries reported in 2007-08.
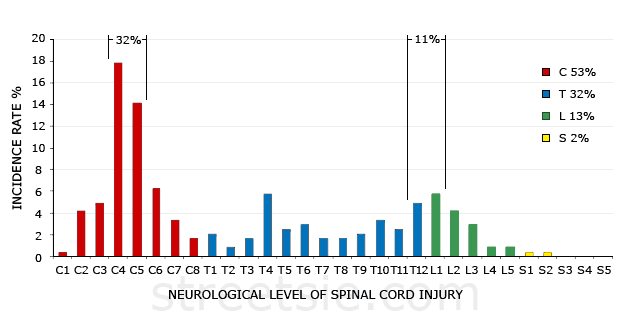
The next most common neurologic level of spinal cord injury is the thoraco-lumbar junction with 11% of cases reporting neurological impairment at T12-L1. Injuries to the thoracic spine accounted for 32% of all injuries reported. The number of thoracic spinal injuries ranged between 64 in 2003-04 to a high of 93 in 2004-05 in Australia. Reports from 2000 to 2010 show an annual average of 31% of all SCI occurred at the thoracic levels T1-T12. Lumbar and sacral injuries make up the remaining cases.
Neurological Category of Spinal Cord Injury
The overall severity of spinal cord injury is measured by a combination of the neurological level of injury (tetraplegia or paraplegia) and extent of injury (complete or incomplete). These are divided into five neurological categories;
- Complete Tetraplegia
- Incomplete Tetraplegia
- Complete Paraplegia
- Incomplete Paraplegia
- Complete Recovery
Approximately 65% of all spinal cord injury cases are diagnosed as incomplete injuries. In 2007-08 a study group of 241 Australian patients with permanent spinal cord injury were diagnosed under the following categories;
- Incomplete Tetraplegia 38%
- Incomplete Paraplegia 27%
- Complete Paraplegia 20%
- Complete Tetraplegia 15%
This distribution of neurological injury is relatively consistent from year to year. Similar results have been found in Europe although a slightly different model appears in the United States where reports show greater proportions of complete SCI cases, mostly attributed to a higher proportion of penetrating gunshot injuries.
excellent report i had injury in c4-5 but uppar body normal but can move legs but cant take weight to stand up. kindly reply some one if this rewalk can help i seen on some websites. but its to pricey and its helpful in quadrapgic or just helpful to paraplegic only. kindly reply, anshuman