Testing Reflexes Redefining Spinal Shock
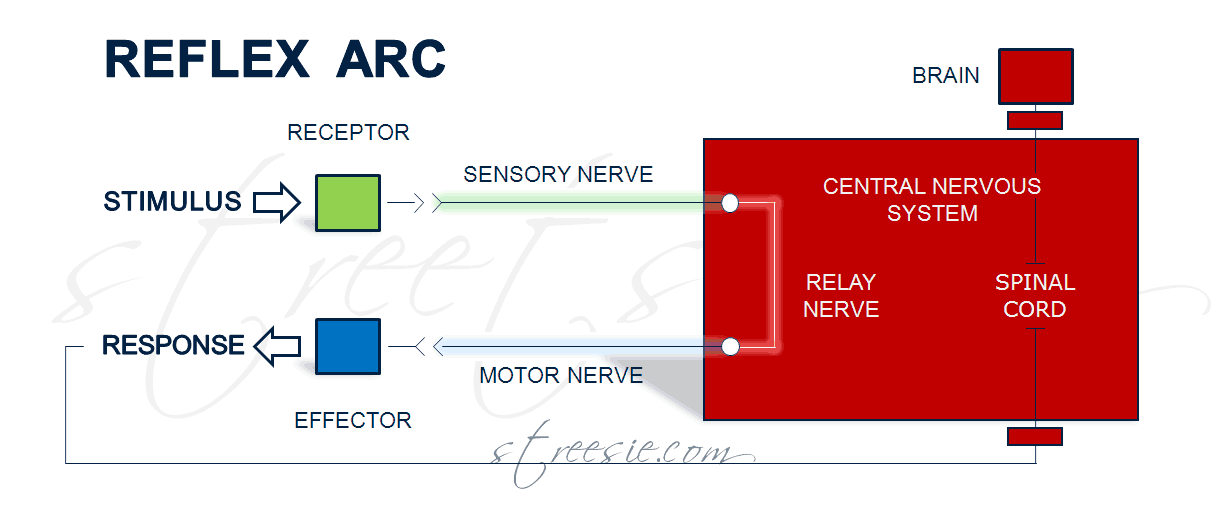
Vital information on the nervous system is gathered by testing reflexes after spinal cord injury. The path reflex neurons follow (the reflex arc) do not rely on intact nerve paths to the brain. They synapse (jump a small gap between nerve ends) in the spinal cord returning along motor nerves to quickly trigger muscles. Impulses travel along these refex arc nerves at 127 mph.
Stimulus to a reflex tendon creates an impulse that travels along sensory nerve axons (long middle section of nerve) to the spinal cord where it returns along motor nerves to trigger a muscle response, without the delay of routing signals via the brain, although (in a healthy spinal cord) the brain will receive motor (muscle) sensory feedback when the reflex arc fires.
There are two types of reflex arc — autonomic (affecting inner organs) and somatic (affecting muscles), — an accurate assessment of reflex arc function determines the location and severity of spinal cord injury, resulting amount of paralysis, and formulates expected long term outcomes. Testing reflexes also gives strong indications whether a spinal cord injury is incomplete or complete.
After severe spinal cord injury paralysis and limited to no sensation below the level of injury is typical, but it is rare to present no reflexes – spinal shock. Almost one third of patients examined within 1-3 hours of injury do present some reflexes. Describing spinal shock as the period following injury during which all spinal reflexes are absent is being phased out.
The evolution of reflexes over several days following spinal cord injury are now considered more relevant to prognosis than the use of the term spinal shock and the presence or absence of reflexes on the actual day of injury.
Reflexes and Corresponding Spinal Cord Nerve Supply Level

- Biceps jerk C5, C6
- Supinator jerk C6
- Extensor digitorum reflex C7
- Triceps jerk C7, C8
- Abdominal reflex T8-T12
- Knee jerk L2-L4
- Ankle jerk L5, S1, S2
- Bulbospongiosus reflex S2-S4
- Anal reflex S5
- Plantar reflex L5-S2
Delayed Plantar Response Reflex
Delayed Plantar Response (DPR) is a reflex present in all patients with complete spinal cord injury. DPR is demonstrated by pressing a blunt instrument firmly from the heel along the lateral (outer) sole of the foot and continuing slowly across the metatarsal heads (where foot bones connect to toes). Following this stimulus the toes flex and relax in delayed sequence. Caution should be taken to not misinterpret the flexion component as a normal plantar response.
Deep Tendon Reflex
Deep tendon (stretch) reflexes provide information on the integrity of the central and peripheral nervous system. Generally, decreased reflexes indicate a peripheral problem and lively or exaggerated reflexes a central one. Deep tendon reflexes are usually absent in complete spinal cord injuries as both peripheral and central nervous systems have been compromised, and conversely are present in the majority of patients with incomplete spinal cord injuries.
Anal and Bulbospongiosus Reflex
Understanding the usefulness of sacral reflex arcs in determining the location and severity of spinal cord injury requires definition of the term bulbospongiosus. Imagine a diamond between your legs (no girls, not that kind of diamond lol), the perineum, a diamond shaped erogenous zone that includes the anus and penis or vagina.
Bulbospongiosus muscles are superficial (surface) muscles of the perineum. In males that includes the base of the penis to halfway up the penis shaft. Its function is to empty the urethra and contributes to erection, ejaculation, and the feelings of orgasm. In females, residing either side of the vagina, bulbospongiosus muscles are responsible for clenching the vagina closed and contribute to clitoral erection and the feelings of orgasm. Both anal and bulbospongiosus reflexes rely on intact sacral reflex arcs.
Anal reflex is an externally visible contraction of the anal sphincter triggered by pin prick. The bulbospongiosus reflex is a similar contraction of the anal sphincter in response to firmly squeezing the penis head or clitoris.
Testing anal and bulbospongiosus reflex arcs aid in distinguishing between upper motor neuron lesions in which the reflex may not return for several days, and lower motor neuron lesions in which the reflex remains abaited unless neurological recovery occurs.
- Upper motor neuron lesion; injury of upper motor neurons are common because of the large amount of cortex occupied by the motor areas, and because motor pathways extend all the way from the cerebral cortex to the lower end of the spinal cord.
- Lower motor neuron lesion; injury of lower motor neurons are less common as they are typically secondary injuries. Lower motor neurons relay the movement instructions provided by upper motor neurons, from spinal cord to the relevant muscles. When the lower motor neurons are damaged the result is muscle weakness, twitching and atrophy.
Conclusion
As a part of primary and secondary initial hospital assessments the testing of reflexes delivers conclusive information relevant in determining the level and completeness of a spinal cord injury. The term spinal shock is being phased out. The evolution of reflexes over several days to weeks following spinal cord injury are considered significant factors in determining long term outcomes.
Resources
- Wikipedia; http://en.wikipedia.org/wiki/Reflex_arc
- Merck Manuals; http://www.merck.com/mmhe/sec06/ch077/ch077c.html
I’D LIKE MORE INFORMATION ABOUT THIS, i HAVE A LOT OF MOVEMENT AND TIGHTNESS.
Good!!! Well Done!!!